Last Updated on: 14th March 2026, 07:21 am
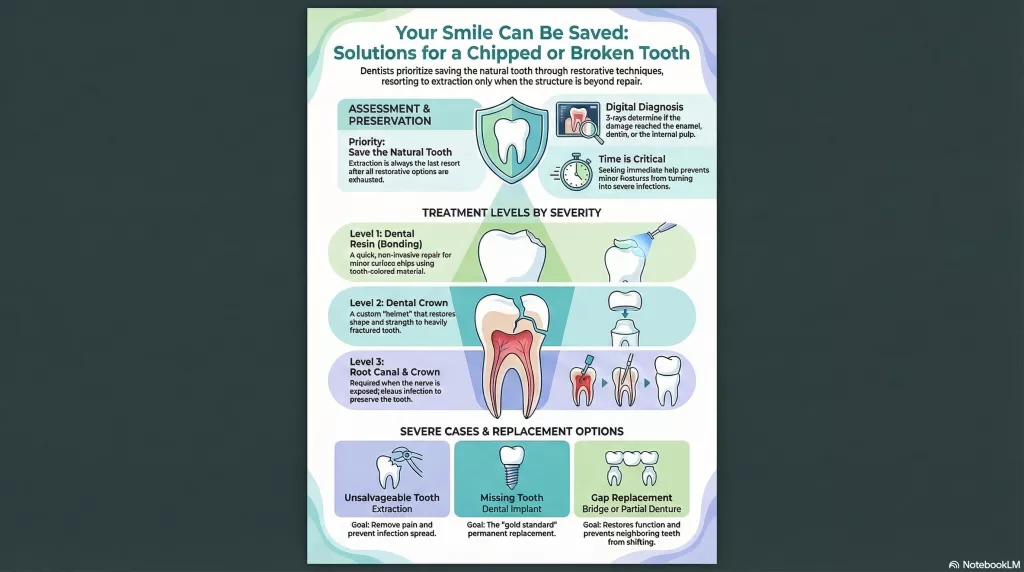
A chipped or broken tooth can almost always be repaired. Treatment depends on how deep the damage goes and may include bonding, a crown, a root canal with a crown, or extraction with replacement options like implants or bridges. A dentist exam with X-rays determines the best solution.
You bit down on something hard. You took a fall. Or maybe you just woke up and felt something wasn’t right. Whatever happened, you now have a chipped or broken tooth, and you need to know: can it be fixed?
Almost always, yes. At Channel Islands Family Dental, we treat broken and chipped teeth every day at our clinics across Ventura County. The treatment depends on how much damage there is, but there is a solution for every level of fracture. Let’s walk you through it.
Table of Contents
ToggleFirst: is this an emergency or can it wait?
Not all broken teeth are the same urgency, and knowing the difference helps you make the right call right now.
Get to a dentist the same day if:
- Your tooth was completely knocked out of its socket
- You have intense, throbbing pain that over-the-counter medication isn’t touching
- Your face, jaw, or gums are visibly swollen
- You have a fever alongside tooth pain, this can mean a spreading infection
- A large portion of the tooth broke off and you can see a yellowish or pinkish interior (that’s the nerve)
You can schedule within a day or two if:
- A small chip broke off with no pain
- You feel a rough edge but the tooth is otherwise intact
- There’s mild sensitivity but no swelling or severe pain
When in doubt, call us. Our team at Channel Islands Family Dental, with offices in Ventura, Oxnard, and Port Hueneme, can help you assess urgency over the phone and get you in fast.
The scenario that can’t wait: when a tooth is completely knocked out
If your tooth came out of its socket entirely, from a sports collision, a fall, or any hard impact, you have a narrow window to save it. This is the one scenario where minutes genuinely matter.
Do this right now:
- Pick the tooth up by its crown, the white part you normally see. Never touch the root.
- Rinse it gently under clean, room-temperature water. No soap, no scrubbing, no drying it off.
- Try to place it back into the empty socket and hold it gently in place. This is the best way to keep it viable.
- If you can’t do that, tuck it inside your cheek, your saliva helps keep it alive. A glass of cold milk works too.
- Head straight to Channel Islands Family Dental. The reimplantation window is 30 to 60 minutes. Don’t stop for anything.
If you make it in time, your dentist can reposition the tooth, stabilize it with a splint, and give it a real chance of reattaching to the bone. If reimplantation isn’t possible, we’ll move straight into discussing your best replacement options.
How your dentist decides what treatment you need

Before any treatment begins, your dentist needs to understand the full picture.
- The dentist checks your tooth and takes digital X-rays, because what you can see on the surface of a broken tooth tells only part of the story. The X-rays reveal how deep the fracture goes, whether the nerve is involved, and whether the root is still healthy. This information helps the dentist choose the right treatment and avoid the wrong one.
- A tooth has three layers: the enamel on the outside (hard and protective), the dentin underneath it (softer, more sensitive), and the pulp at the very center (where the nerves and blood vessels live). Treatment choices follow this anatomy exactly. The deeper the fracture, the more involved the treatment, but also the more important it is to act.
At our Newbury Park and Santa Paula offices, as at all Channel Islands Family Dental locations, this diagnostic process is thorough, fast, and explained to you in plain language every step of the way.
What will the dentist do to fix a broken tooth?
This is the most important part. Treatment is chosen based on how deep the damage goes.
Dental bonding: when it’s a minor chip
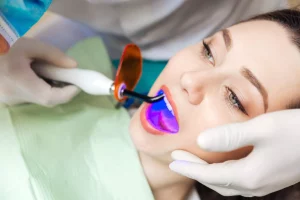
Your dentist applies a tooth-colored resin directly onto the chipped area, shapes it to match your tooth, and hardens it with a special light. It’s quick, usually done in one visit, no shots needed, and the result looks completely natural.
Bonding typically lasts 5 to 10 years with normal care, and all Channel Islands Family Dental locations offer it as a same-day service in most cases.
Dental crown: when a large piece has broken off
A crown is a custom cap that covers the entire tooth. Think of a crown as a custom helmet for your tooth: it fits precisely over everything that remains above the gumline, restoring the tooth’s full shape, strength, and appearance in one restoration.
Here’s what the process looks like:
- Visit one: Your dentist shapes the remaining tooth to make room for the crown, takes impressions (or digital scans), and places a temporary crown to protect the tooth while your permanent one is being made.
- One to two weeks later: Your permanent crown — typically made of ceramic or porcelain — is placed and checked for fit, bite, and color. When it’s right, it’s cemented in permanently.
- Before the final crown is placed some patients need one or more additional visits to check fit, bite and color. This helps make sure the crown looks natural and fits comfortably before it is permanently placed.
Modern crowns are remarkably lifelike. Most people can’t tell the difference between a crown and a natural tooth, not even the patient. With good care, a crown can last 10 to 15 years or longer.
Root canal treatment + crown: when the nerve is involved
If the break reaches the nerve inside the tooth, you’ll likely feel a deep, throbbing ache, and a root canal is needed first.
- Your dentist removes the damaged nerve tissue, cleans the inside of the tooth, and seals it.
- Then a crown is placed on top for protection.
Root canal treatment is available at all Channel Islands Family Dental clinics, including our offices in Oxnard and Ventura. And if dental anxiety is a concern for you, ask our team about sedation options, nitrous oxide and oral sedation are available to make your experience as relaxed as possible.
Extraction and replacement: when the tooth can’t be saved
When the fracture is too deep or decay destroyed too much, extraction is sometimes the only option.
- Extraction is always a last resort at Channel Islands Family Dental; we’ll look for every viable alternative first.
- But when it is necessary, the procedure itself is much more straightforward than most patients expect.
- With proper anesthesia, you’ll feel pressure but not pain.
What happens after an extraction matters just as much as the extraction itself. Leaving a gap in your smile isn’t just cosmetic, over time, neighboring teeth can shift, the jawbone beneath the gap can deteriorate, and your bite can be affected. That’s why we always discuss replacement options right away.
Replacing a tooth you lost
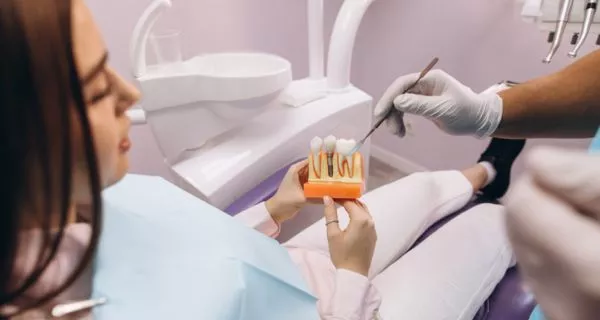
After an extraction, or after losing a tooth from an injury, you have great options:
- Dental implant: A titanium post is placed in the jawbone and topped with a porcelain crown. It looks, feels, and functions like a real tooth. With proper care, it can last a lifetime. This is the gold standard.
- Dental bridge: A fixed restoration anchored to the teeth on either side of the gap. No surgery, done in a couple of visits, long-lasting.
- Partial denture: A removable option when fixed restorations aren’t the right fit. More affordable, still effective.
Your dentist will explain which option suits your situation, health, and budget, no pressure, just honest guidance.
Taking care of your tooth after treatment
Whether you got a simple bonding or a full crown with a root canal, a little attentiveness after treatment goes a long way:
- Avoid very hard or sticky foods on the treated tooth for a few days
- Brush and floss as usual, just be gentle around the restored area
- If you grind your teeth, ask your dentist about a custom night guard, it protects your restoration and your other teeth
- Keep your follow-up appointments
- Call us right away if something doesn’t feel right
A broken tooth can shake your confidence. It can make you self-conscious about eating, talking, and laughing. But here’s the truth that years of restorative dentistry have taught us: there is almost always a solution. And the sooner you come in, the better that solution will be.
Don’t sit on a broken tooth and hope it gets better on its own, it won’t. But come see us, and we’ll show you exactly what’s possible.
Channel Islands Family Dental is here for you, with offices across Ventura County in Ventura, Oxnard, Port Hueneme, Newbury Park/Thousand Oaks, and Santa Paula. Whether it’s an emergency today or a repair you’ve been putting off, we’ll take care of you.
Call us or book your appointment online at https://cidentist.com/, we’re ready when you are.
FAQs
Voice and Search Snippets (Q&A)
References
1. Dunkin, M. A. (2025, January 20). Repairing a chipped or broken tooth. WebMD. https://www.webmd.com/oral-health/repairing-a-chipped-or-broken-tooth
2. Patel, J. (2022). Dental Trauma: A Practical Guide to Diagnosis and management. Dental Traumatology, 38(3), 250–251. https://doi.org/10.1111/edt.12747
3. Patnana, A. K., Brizuela, M., & Kanchan, T. (2025, February 17). Tooth fracture. StatPearls – NCBI Bookshelf. https://www.ncbi.nlm.nih.gov/books/NBK551650/
4. Watson, S. (2025, November 18). How to care for a cracked or broken tooth. Verywell Health. https://www.verywellhealth.com/toothache-relief-from-a-cracked-or-broken-tooth-1059317
5. WebMD. (2024, October 14). Handling dental emergencies. https://www.webmd.com/oral-health/handling-dental-emergencies