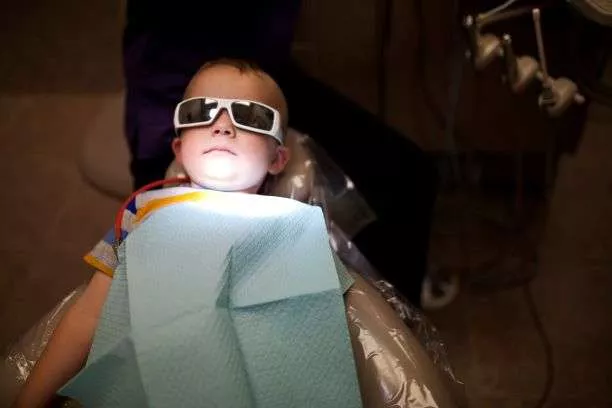
Dental care is the number one unmet health issue in children with special needs. According to the American Psychiatric Association , across all economic sectors, children with special needs are almost twice as likely to go without dental care as their peers without special needs.
Although autism is not characterized by any specific pathological condition at the oral health level, the autistic patient usually presents with more oral disease than patients without this syndrome of similar age. In addition, it is associated with a higher prevalence of problems related to harmful habits, such as bruxism, self-injury of the tongue, lips, and gums, biting, and the like due to the tendency to self-injury that these patients may present.
ORAL MANIFESTATIONS OF AUTISM SPECTRUM DISORDER (ASD)
People with autism manifest a large number of manias and harmful habits related to the mouth:
- Some may exhibit self-flagellation behaviors such as hurting their gums, biting their lips, or causing ulcerations.
- Some drugs for anxiety, behavioral problems, schizophrenia, and manic episodes, and epilepsy, among others, produce side effects that affect salivary secretion, decrease it, and produce dry mouth or xerostomia, which results in an increased risk of caries and gum problems such as hyperplasia.
- Poor oral hygiene due to the difficulty of some children/caregivers to implement home care.
As a consequence of these harmful habits, malocclusion occurs more frequently, and problems in the main functions of the stomatognathic system are present: phonation, swallowing, and chewing.