Last Updated on: 5th December 2024, 10:31 am
What is gingivitis?
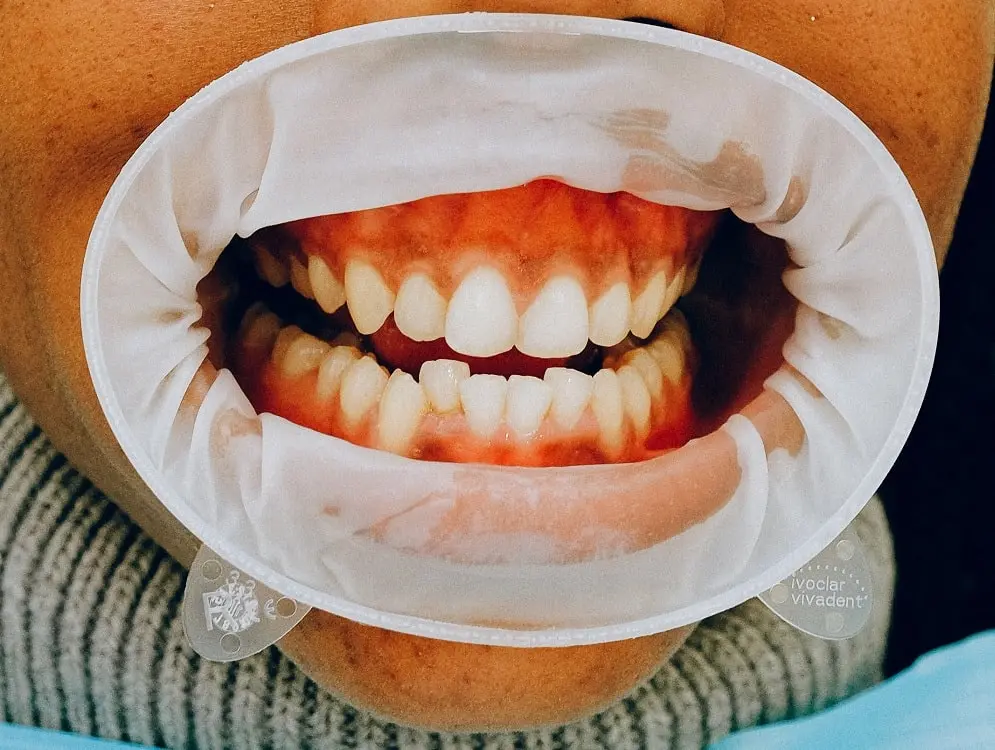
- Red, swollen, and tender gums
- Bleeding gums, especially while brushing or flossing
- Bad breath
- Receding gums
- A change in the color of gums from pink to dusky red
- Gingivitis is a reversible condition that can be treated and managed with proper oral hygiene practices such as brushing twice a day, 7. flossing, and regular dental checkups and cleanings.
What is periodontitis?
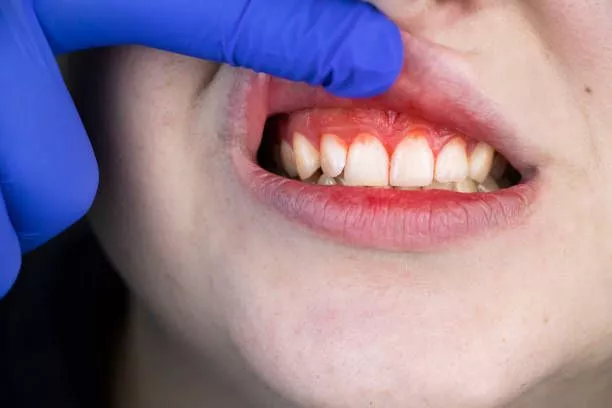
- Persistent bad breath
- Receding gums
- Deep pockets between the teeth and gums
- Loose or shifting teeth
- Changes in the way teeth fit together when biting down
- Painful chewing
- Sensitive teeth
- Periodontitis is a severe condition that requires prompt treatment by a dentist or periodontist. Treatment options may include scaling and root planing, antibiotics, surgery, and other procedures to help restore gum and bone health.
Key differences: gingivitis or periodontitis
- Although Gingivitis and Periodontitis share some symptoms, there are significant differences between the two conditions. Here are some of the most significant differences:
- Gingivitis is reversible, while Periodontitis is not. Gingivitis can be treated and managed with proper oral hygiene practices, whereas Periodontitis requires more aggressive treatment to prevent further damage.
- Gingivitis affects only the gums, while Periodontitis can affect the gums, bone, and other structures that support the teeth. In Periodontitis, the bacterial infection has spread beyond the gums, leading to more severe damage.
- Gingivitis is a milder form of gum disease, while Periodontitis is a more advanced stage. If left untreated, Gingivitis can progress to Periodontitis.
Gingivitis or periodontitis: Prevention
- Brushing your teeth at least twice a day with fluoride toothpaste
- Flossing daily to remove plaque and food particles from between the teeth and under the gum line
- Using an antiseptic mouthwash to help kill bacteria and freshen breath
- Eating a balanced diet and avoiding sugary and acidic foods and beverages that can contribute to tooth decay and gum disease
- Visiting your dentist
Conclusion
Contact us
If you have any questions about gingivitis or periodontitis and other topics, you can contact us at Channel Islands Family Dental as well as our page on Facebook. We look forward to your visit and we will make a timely diagnosis. Our dentists in Oxnard, Santa Paula, Ventura, Newbury Park, and Port Hueneme will be able to guide you toward the best treatment to take care of your health and give you back your best smile.
Bibliography
- 1″Gingivitis.” Mayo Clinic, Mayo Foundation for Medical Education and Research, 23 Apr. 2021, www.mayoclinic.org/diseases-conditions/gingivitis/symptoms-causes/syc-20354784.
- “Periodontitis.” Mayo Clinic, Mayo Foundation for Medical Education and Research, 6 May 2021, www.mayoclinic.org/diseases-conditions/periodontitis/symptoms-causes/syc-20354473.
- Newman, Michael G, and Henry H Takei. Carranza’s Clinical Periodontology. 13th ed., Elsevier, 2018.