Last Updated on: 21st October 2024, 01:20 pm
Periodontitis in the early stage is a disease that affects the gums caused by the accumulation of bacterial plaque. It is a more advanced stage of gingivitis and more destructive since it damages the soft tissue that surrounds the tooth and, if not removed, can also destroy the bone that supports the teeth, causing them to loosen or be lost.
This disease affects between 15% and 20% of adults between 35 and 44 years old, according to the World Health Organization. It is not common in children; however, it can occur frequently during adolescence.
What is periodontal disease or periodontitis?
To understand the development of the disease, it is important to know its different phases:
- Gingivitis: It is the inflammation of the gum, which occurs due to the accumulation of bacterial plaque caused by poor hygiene habits.
- Initial periodontitis: It occurs when the accumulation of plaque persists over time.
- Moderate periodontitis: It is characterized by gum recession and the destruction of part of the bone that supports the tooth.
- Advanced periodontitis: It is the almost total destruction of the bone that supports the tooth. At this point, there may be mobility of the teeth, and they are more prone to loss.
What is initial periodontitis?
As previously mentioned, periodontitis is a chronic inflammation that occurs in the gums when there is a buildup of bacterial plaque. In this stage, the gums may appear to be receding or diminishing in appearance. The accumulated plaque hardens and becomes calculus, also known as tartar. At this point, the bone begins to be affected by the bacteria.
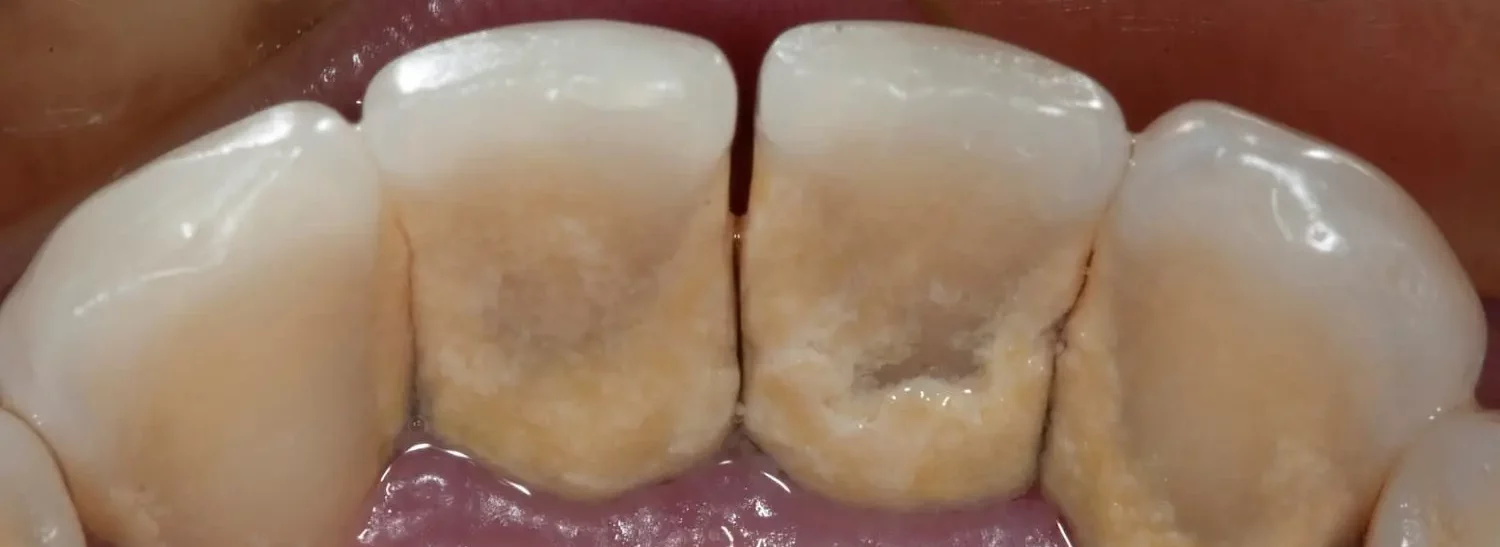
What are the symptoms of periodontitis in the early stage?
When periodontal disease begins, the symptoms can be very subtle and silent, especially in smokers, where the effects of tobacco on gum vascularization can cause the disease to start inadvertently.
At this point in the disease, symptoms are minimal and can be reversed if diagnosed and treated early. Some symptoms include:
- Inflammation and color change in the gums: When there is inflammation, the gums turn a deep red or violet color.
- Bleeding: A common symptom of periodontal disease is bleeding upon any stimulation, such as brushing.
- Bad breath or halitosis: This is caused by bacteria present in the mouth.
- Tooth sensitivity: Not a common symptom, but it can occur when the gums recede and the tooth root is exposed, causing sensitivity to certain stimuli such as sweet and acidic foods or changes in temperature.
Once the disease has started, the most important sign is bone loss. This sign is not easy to see, so it must be diagnosed by a periodontal specialist dentist. The dentist performs a clinical examination with a specialized instrument called a periodontal probe, which measures the gums. When there is a disease, the gums have a separation of the teeth called periodontal pockets, which contain bacteria that can worsen the disease.
Bleeding upon brushing and flossing may also occur, and the initial stages of bone loss may begin. To confirm bone loss, the dentist may use diagnostic images such as periapical radiographs.
What can cause initial periodontitis?
All people have a variety of bacteria in their mouth, most of which are completely harmless depending on the person’s health condition and by controlling their growth. However, the accumulation of bacterial plaque brings in bacteria that are not harmless, but instead are harmful. These bacteria can grow and become accumulated in the teeth.
When there is no proper brushing, or when flossing is not a habit, bacterial plaque can harden into dental calculus. It is also important to consider some external factors that can help accelerate the development of the disease:
- Smoking: This is a very common habit among young people. In addition to pulmonary problems, smoking can increase gum inflammation without any apparent symptoms.
- Type 2 diabetes.
- Obesity.
- Hormonal changes in women, especially during menstruation, pregnancy, and menopause.
- Diseases that affect the immune system, such as HIV or leukemia.
- Medications that reduce saliva production.
- Poor nutrition.
- Xerostomia (low saliva production)
What is the treatment for periodontitis in the early stage?
It is important to diagnose and treat the disease early to avoid future complications, especially in people susceptible to developing it. The treatment should aim to eliminate bacterial deposits in the teeth and gums.
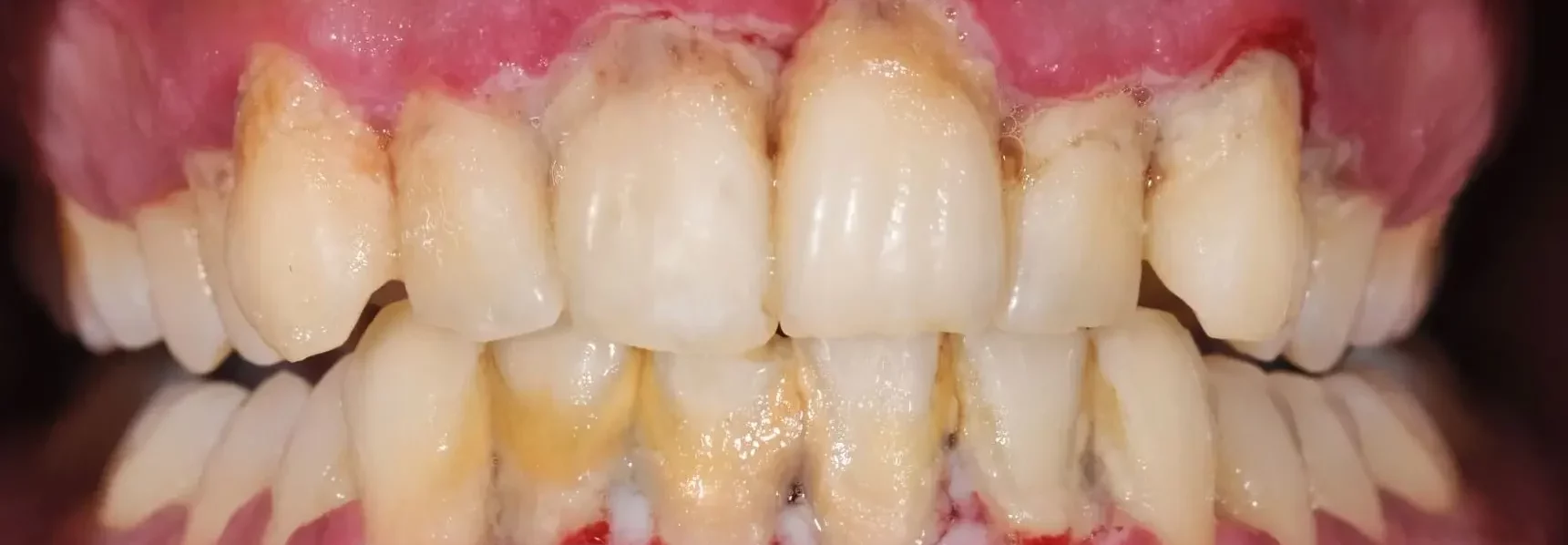
Possible treatments for initial periodontitis are:
- Oral hygiene practices: It is important to regularly visit the dentist to learn brushing techniques and the proper use of dental floss.
- Scaling and root planing: This treatment should be performed by a specialist dentist. It involves the removal of calculus and bacterial plaque using specialized instruments. It can be a little uncomfortable or painful, so it should be done under local anesthesia.
- Antibiotics: In some cases, it may be necessary to complement the treatment with antibiotics to help decrease persistent infections in the gums. The antibiotics can be a mouthwash, topical gel, or oral tablet.
- Follow-up appointments: It is important to attend the follow-up appointments scheduled by the dentist to prevent disease recurrence or complications with persistent infections.
- Surgery: If the inflammation persists, the dentist may recommend surgery to remove the accumulated bacteria and calculus in the teeth and gums. This procedure involves lifting the gums under local anesthesia. After cleaning the affected area, it is closed with sutures. Generally, the disease disappears after this procedure, but it is the last option to consider.
How to prevent periodontal disease?
Oral hygiene is important to prevent periodontal disease, whether at a professional level or at home care. Good hygiene is essential for the success of dental treatments:
- Correct brushing technique: this can be indicated by the dentist and will be according to each patient’s needs.
- Brushing at least three times a day: it is recommended to brush three times a day after meals. If you cannot brush three times due to work or time constraints, you should ensure that brushing is done in the morning and at night as this is when bacteria are most active in the mouth.
- Avoid hard bristle brushes: hard bristle brushes can be rough on the gums. Use brushes with medium or soft bristles.
- Use appropriate toothpaste: the dentist will indicate the type of toothpaste that should be used according to each person’s needs.
- Electric brush: electric brushes can be used, especially in people with mobility difficulties.
- Interdental hygiene: the use of dental floss is important to complement brushing. Dental floss reaches places where the brush cannot reach.
- Healthy lifestyle: having good habits and lifestyles are essential to maintaining not only oral health but also general health.
It is necessary to regularly consult the dentist and undergo professional cleanings to avoid the development of periodontitis in the early stage.
Contact us
If you have any questions about this or other topics, you can contact us at Channel Islands Family Dental as well as our page on Facebook. We look forward to your visit and we will make a timely diagnosis. Our dentists in Oxnard, Santa Paula, Ventura, Newbury Park, and Port Hueneme will be able to guide you toward the best treatment to take care of your health and give you back your best smile.
Bibliography
- Bascones Martínez A, F. R. (December 3, 2005). Advances in Periodontics and Oral Implantology. Retrieved from Las enfermedades periodontales como infecciones bacteriana. https://scielo.isciii.es/scielo.php?script=sci_arttext&pid=S1699-65852005000300004
- C. Rolando Sánchez Artigas, R. J. (February 26, 2021). Correo cientifico medico. Retrieved from Risk factors of periodontal disease. https://revcocmed.sld.cu/index.php/cocmed/article/view/3585/1892
- Carla María García San Juan, R. D. (June 23, 2021). Redalyc. Retrieved from The new classification of periodontal and peri implant conditions and diseases from an evolutionary perspective: https://www.redalyc.org/journal/1800/180069886013/html/
- Castro-Rodríguez, Y. (April 01, 2018). Clinical journal of periodontology and oral implantology. Retrieved from Periodontal disease in children and adolescents. Case report. https://www.scielo.cl/scielo.php?script=sci_arttext&pid=S0719-01072018000100036
- Clinica mayo. (May 05, 2020). Clinica mayo. Retrieved from Periodontitis. https://www.mayoclinic.org/es-es/diseases-conditions/periodontitis/symptoms-causes/syc-20354473
- Maria V. Velez-Sanchez, F. G.-F. (June 20, 2017). Revista cientifica. Retrieved from Clinical protocol and treatment of patients with Periodontitis: Case Report