Last Updated on: 17th February 2026, 09:32 am
Normally in the mouth, it is kept in balance with different types of microorganisms (bacteria, fungi, and some viruses), however, these generally do not manifest when we maintain adequate oral hygiene. But, when we do not brush our teeth properly, we have a diet that is high in carbohydrates, sugars, carbonated drinks, acidic foods, or foods that are corrosive to tooth enamel, we do not use dental floss and we do not make regular visits to the dentist; An environment conducive to bacterial and fungal growth is generated, since the pH of the saliva changes and dental plaque accumulates under the gums, being a favorite environment for the growth of these microorganisms.
Therefore, gum diseases come, bad breath (Halitosis), and depending on how advanced this infection is, it is possible to observe red, bleeding and inflamed gums, which are initial symptoms of gingivitis and one of the classifications associated with gingivitis is trench mouth, which we will explain in the document.
What is trench mouth?
It is an acute infection of the gums, the most severe form of gingivitis and advanced, meaning it can come on quickly and cause serious damage to your gums and teeth.

Within the social context it is known as a trench mouth; however, clinically it has several diagnoses such as: acute necrotizing ulcerative gingivitis (ANUG), Vincent’s disease or Vincent’s stomatitis. It manifests clinically with bleeding gums, inflammation, pain followed by ulceration between the teeth and gum tissues; which makes this condition quite painful, and is associated with initial or pre-existing gingivitis as a result of poor oral hygiene and that was not treated in time.
Its name trench mouth was given by the soldiers who during the First World War presented these serious oral health problems, since, due to lack of access to dental care and hygiene during battle, they developed very serious gum diseases.
This rare condition is commonly identified in adolescents and young adults; however, in some underdeveloped countries or populations with a very high poverty rate, it can be seen, since, added to the lack of access to health products and dental care, there is also a deficiency in food and living conditions. It is possible that in patients whose immune system is affected by some disease or health condition, it occurs more frequently.
What causes trench mouth?
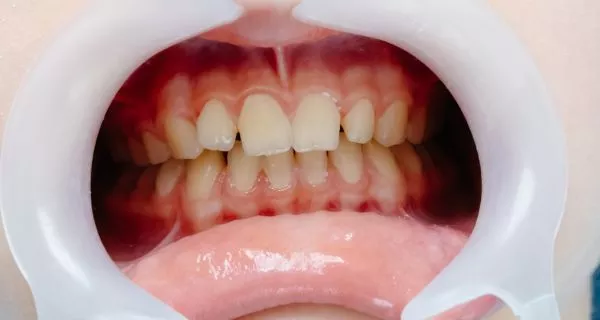
This condition results from infection of the gums by an excess of harmful bacteria. If left untreated, it can get worse and some studies indicate that the mechanisms by which it develops are not well understood. However, poor oral hygiene is the main cause, but there are other risk factors that can increase the its likelihood:
- Poor oral hygiene
- High levels of stress
- Infection of the mouth, throat, or teeth
- Poor diet, vitamin deficiency, and minerals
- Smoking
- Diabetes
- Pre-existing gingivitis
- Having lesions on the gums
- Alcohol abuse
- Weakened Immune system (cancer or other diseases that require immunosuppressants)
- HIV/AIDS
This infection is more common in people aged 15-35 years and damages the gum tissues of those who suffer from it and may cause loss of dental pieces.
What are the symptoms of trench mouth?

It is a severe acute form of gum disease, characterized by rapid deterioration of gum tissue and rapid progression of infection. The main symptoms include:
- Extreme bad breath
- Ulcers: crater-shaped sores between the teeth and gums
- Trench mouth tongue
- Fever
- Pain
- GumsRed and swollen gums
- that bleed on slightest contact
- Bad taste in the mouth
- Yellow-white or gray membrane covering the ulcerated papillae
- Swollen lymph nodes around the head, neck, or jaw
- Fatigue
- Severe bleeding from the gums, in response to brushing
Complications:
- If left untreated, it can lead to rapid destruction of gum tissue. gums and spread to other tissues, such as the cheeks, lips, or jaw bones.
- Untreated trench mouth can cause weight loss, dehydration, and infection that can spread, in some very severe cases it can cause oral gangrene.
- Gum surgery is important to treat craters, if not addressed properly in time it could lead to tooth loss.
How is trench mouth diagnosed?
- Medical history, including diet and general habits
- Investigation for the presence of any health conditions that weaken the immune system
- Dental history, with particular attention to symptoms of pain and pre-existing gingivitis
- Check for swollen glands in the area of the head and neck
- Check the oral cavity for signs of infection and swelling
- Do blood tests to check for certain bacteria associated with it.
- X-rays to assess whether the infection has spread to the bone.
How do you get rid of trench mouth?

The main goal of treatment for trench mouth will be to cure the infection and relieve symptoms. For this there are four stages on how to manage it:
Stage 1: Control the progression of the disease and relieve symptoms of discomfort and pain.
- Elimination of dead or affected tissues from diseased areas using: mouth rinses periodically with: chlorhexidine, hydrogen peroxide (hydrogen peroxide), salt water or instruments that can help this such as ultrasound.
- Use of antibiotics when there is fever or swollen glands due to bacterial infections. This will depend on how advanced it is and in some cases it is started with an antibiotic, but if it does not improve, a culture should be performed and the possible sensitivity of the bacteria to any of these antibiotics should be evaluated.
- Use of analgesics: depending on the pain or discomfort, you can access over-the-counter ones or if they must be prescribed the treatment will be indicated by your dentist.
Stage 2: Treatment of pre-existing conditions such as gingivitis
- Professional cleaning of teeth and gums, scaling and root planing of teeth, with the aid of local anesthesia
- Instructions and guidelines for patients to maintain good nutrition, fluid intake, smoking cessation habits and good oral hygiene.
- Good oral hygiene: Brushing twice a day, flossing, mouthwashes, and regular cleanings by a dentist.
Stage 3: Surgical procedures
- This stage involves surgery on the gums to fill in the craters between the teeth.
- The decision to perform surgery should be limited to those cases in which, once the acute phase of the disease has been resolved and with correct plaque control by the patient, it could be considered that the remaining gingival structure makes proper hygiene difficult or impossible.
- In the surgical treatment plan and in the design of the incisions, we must be extremely careful to avoid the removal of excessive healthy tissue for the normalization of the gingival structure.
- The minimum waiting time for the resolution of the case through surgery should be one month after the disappearance of the acute infection
Stage 4: Maintenance and support
- Involves long-term follow-up with good oral hygiene and regular check-ups.
- Improve quality of life by exercising to reduce stress and eating a balanced, healthy diet.
Treatment generally involves a combination of strategies to help prevent the disease from getting worse. Your dentist may recommend medications, surgery, or other options to help treat it.
What antibiotics are used for trench mouth?
The most used and prescribed for oral administration (by mouth), are the following according to the order:
- Penicillin
- Metronidazole
- Amoxicillin
- Erythromycin
- Tetracycline
Depending on the diagnosis, the dose, frequency and days of treatment vary, which will be defined by the dentist or specialist. If the infection has spread to other parts of the body, you may require antibiotic management systemically or intravenously (that is, through the vein)
How long does it take to get rid of trench mouth?

With proper treatment, relief of symptoms occurs within a few days, and it can usually be cured within weeks. It is a very serious and acute infection that requires treatment and will not go away on its own. With the right treatment it is possible that it will be solved or cured since not all treatments are effective, here are some examples:
- The root cause of the infection was NOT eliminated by treatment
- Tissue remains, infected or dead after treatment.
- It presents health conditions that do not favor recovery and the healing becomes slower or more difficult.
- The patient does not follow the recommendations and adequate treatment. In relation to oral or surgical treatment and good oral health.
- Health conditions that affect the patient and their oral health.
Ways to prevent
Our dentists often educate our patients on the benefits of brushing and flossing regularly. It can be easily prevented by maintaining good oral hygiene with regular checkups for signs and symptoms of gingivitis.
It is also important to maintain good overall health by resolving stress, sleeping well, eating good and nutritious food, and giving up bad habits like smoking to build a strong immune system to fight off various infections.
If you have any questions about this or other topics, you can contact us at Channel Island Family Dental as well as our Facebook page. We look forward to your visit and we will make a timely diagnosis. Our dentists in Oxnard, Saint Paula, Venture, New Bury Park , and Port Hueneme will be able to guide you towards the best treatment to take care of your health and give you back your best smile.
Bibliography
- Robles Raya P, Javierre Miranda AP, Moreno Millán N, Mas Casals A, de Frutos Echániz E, Morató Agustí ML. Management of odontogenic infections in primary care consultations: antibiotic? [Management of odontogenic infections in Primary Care: Antibiotic?]. Attention Primary. 2017Dec;49(10):611-618. Spanish. doi: 10.1016/j.aprim.2017.05.003. Epub 2017 Jul 25. PMID: 28754576; PMCID: PMC6876037. Accessed on Sep 28, 2022. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6876037/
- Ubertalli, J. Acute Necrotizing Ulcerative Gingivitis (ANUG). Merck Manual (Internet). Updated Sep, 2022, (Accessed Sep 28, 2022). Available in: https://www.merckmanuals.com/professional/dental-disorders/periodontal-disorders/acute-necrotizing-ulcerative-gingivitis-anug
- Kapner, M; Zivie, D. National Library of Medicine, Medline Plus (Internet). Updated on Jan 24, 2022; (Accessed on Sep 28, 2022). Available in: https://medlineplus.gov/ency/article/001044.htm
- Drugs.com. (Internet). Updated on Aug 31, 2022; (Accessed on Sep 28, 2022). Available in: https://www.drugs.com/cg/trench-mouth.html
- Cleveland Clinic medical professional. Cleveland Clinic (Internet). Updated Jul 21, 2022; (Accessed on Sep 28, 2022). Available at: https://my.clevelandclinic.org/health/diseases/17776-trench-mouth
- Krans, B., Frank, C. Healthline (Internet). Updated Jul 21, 2022; (Accessed on Sep 28, 2022). Available at: https://www.healthline.com/health/trench-mouth
- Coelho, S., Vincent, C. What You Should Know. Verywellhealth (Internet). Posted on Feb 22, 2022; (Accessed on Sep 28, 2022). Available in: https://www.verywellhealth.com/trench-mouth-5218403