Last Updated on: 20th February 2026, 10:15 am
Tooth infection spreading to the bone has multiple causes, such as genetic conditions, having a disease that compromises the immune system and weakens it, metabolic diseases such as diabetes and dental extraction, or gum disease not treated on time.
When oral hygiene is inadequate, infections may develop due to the formation of dental plaque. If not removed, it produces an environment conducive to bacterial growth, which generates acids from the metabolic process and triggers gingivitis, which subsequently aggravates periodontitis. Likewise, if any teeth are removed, added to poor oral hygiene, infections quickly develop and are exacerbated c through a direct channel to the bone.
Stages in which an abscess develops
An abscessed tooth is an infection caused by bacteria entering the center of the tooth (the pulp), which can spread from the tooth’s root to the bone. Generally, it manifests as a pocket of bacterial pus formed around the tooth, affecting other teeth. Three types of infections occur before reaching the bone:
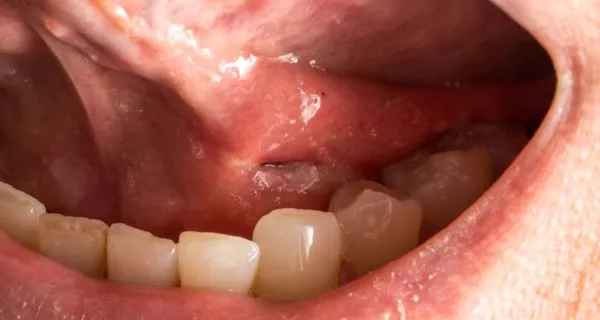
- Gingival: An infection that develops in the gums. It does not affect the tooth or the bone structure.
- Periapical: An infection that forms at the tip of the root. Bacteria spread to the interior of the tooth due to a fracture or caries, come into contact with nerves and blood vessels in the pulp, and spread to the bone, producing the abscess.
- Periodontal: A condition that starts in the bone and the tissues that support the teeth, ultimately resulting in periodontitis or gum disease.
Causes of Tooth Infection

Tooth infection spreading can occur from caries to a dental fissure, accompanied by poor oral hygiene allowing the entry of bacteria. The usual causes are:
- Severe dental caries: A cavity or caries is the destruction of the hard tissue of the tooth surface caused by the decomposition of sugars created by bacteria generating acids that affect the enamel.
- Broken, chipped, or cracked teeth: Bacteria easily enter the pulp through any opening.
- Gum disease (periodontitis): Inflammation of the tissues around the tooth, the product of infection, and as bacteria progresses as they reach deeper tissues.
- Injury to the tooth: Trauma could injure the pulp, and even if there is no crack, it makes it more susceptible to infection.
- A dental extraction (exodontia): Extraction of a tooth with no management of antibiotics or not followed with good dental hygiene allows bacteria to penetrate internal tissues.
- Dental implant: The excessive use of cement in dental implants during the insertion of a prosthesis can minimize bone recovery and bone cell generation, causing inflammation and black areas triggered by the accumulation of material external to the bone.
The above can be caused by:
- Poor dental hygiene (not brushing at least twice a day and flossing)
- A diet rich in sugars and processed flours (cakes, cookies, scones or desserts, soft drinks, sweets)
- Xerostomia or dry mouth, caused by age or some medications (saliva decreases and protection against bacteria is lost)
- Smoking (increased chance of getting infections)
- A weakened immune system (HIV, Diabetes, lupus, arthritis, among others) cannot fight efficiently against bacteria.
Signs of a tooth infection spreading to the bone
- Sensitivity to pressure in the mouth
- Fever
- Taste unpleasant
- Stabbing pain in the jaw, which can spread to the ear and/or neck on the same side as the tooth
- Pain in the area
- Pain that worsens when lying down
- Swelling of cheeks and face
- Purulent discharge from the gums

When the tooth infection spreading starts to develop in other body parts, the symptoms could be:
- Intense or severe headache
- Fatigue
- Dizziness
- Redness of the skin
- Perspiration
- Shaking chills
- Swelling that makes it difficult to open the mouth, preventing eating and breathing
- Darker urine
- Confusion
- Increases the rate of breathing
- Fast pulse
- Diarrhea
- Vomiting
- Droopy eyelids
- Double vision
Do not wait to consult a specialist if any manifest. To emergency medical attention as soon as possible
Osteomyelitis (Mandibular Necrosis)
Osteomyelitis arises as a consequence of a chronic periapical infection or pathologies that obstruct blood flow, leading to bone death and necrosis. Classification is according to time, nature, and characteristics:
- Acute suppurative osteomyelitis: Characterized by intense pain, inflammation, sensitivity, increased temperature, mobility of the teeth involved in the area of the osteomyelitis, and pus secretion.
- Chronic suppurative osteomyelitis: The symptoms are similar and a little less intense, but there may be fistulas, where pus comes out with bone particles detached from the bone. It is generally asymptomatic since the infection is encapsulated in a specific site, isolating the rest of the bone.
- Chronic focal sclerosing osteomyelitis: This condition is frequent in the younger population. It develops in a specific place in the bone with very little inflammation and is asymptomatic.
- Chronic diffuse sclerosing osteomyelitis: It can manifest at any age; however, it is more frequent in older adult patients. Its origin is unknown, but it appears to be caused by a weakened immune system.
Diseases that may appear and treatment
Dental infections can be treated easily and promptly; however, when left untreated, there is a risk of developing
- Osteomyelitis: Infection of the bone surrounding the tooth
- Cavernous sinus thrombosis: Infection of the blood vessels within respiratory structures such as the paranasal sinuses
- Cellulitis: Skin infection
- Parapharyngeal abscess: Abscess at the back of the mouth in the pharynx.
- Sepsis: A serious medical infection in which the immune system reacts strongly to the infection
- Endocarditis: The infection travels to the heart through contaminated blood vessels
- Bacterial meningitis: Infected blood vessels and nerves carry the infection to the brain
It is possible that before diagnosing or starting any type of treatment, your dentist may carry out certain diagnostic tests to properly guide treatment management. Some examples are X-rays, computed tomography, inspection at the site of infection, and/or thermal tests to identify gum sensitivity.
The infection will not go away on its own. Here are some treatment strategies:
- Root canal treatment or endodontics: Root canal or other alternatives will eliminate the infection and save the tooth if it has not yet reached the bone. The infected pulp of the tooth is removed, and the space is filled. The tooth is not lost, usually in mature teeth. In a few days, it should return to normal, and the treated tooth will last a lifetime.
- Incision and drainage: Your dentist will need to make a small incision (cut) in the abscess to drain the pus. Sometimes a small rubber band is placed to keep the incision open for drainage to continue.
- Tooth extraction: Sometimes, it is not possible to save the tooth; therefore, your dentist will remove it and all the tissue affected by the infection.
- Medications: When the infection is not advanced, management with antibiotics is possible; however, if the infection is already an abscess, your dentist will opt for another treatment but may indicate antibiotic treatment as a long-term method to eliminate the infection, preventing it from spreading further. Depending on how advanced it is and what type of bacteria is present, it will require management with natural antibiotics or other forms of medication, or in more serious cases, it will be done in a hospital intravenously.
To have a beautiful and healthy smile, it is important to seek the advice of a professional with experience in this type of disease. They will provide adequate treatment or direct you to a specialist.
Contact us
If you have any questions about this or other topics, you can contact us at Channel Island Family Dental as well as our Facebook page. We look forward to your visit, and we will make a timely diagnosis. Our dentists in Oxnard, Saint Paula, Ventura, Newbury Park, and Port Hueneme will be able to guide you toward the best treatment to take care of your health and give you back your best smile.
Bibliography
1. Souza LN, Souza ACRA, de Almeida HC, Gómez RS, López Alvarenga R. Chronic suppurative osteomyelitis in the upper jaw: report of a clinical case. Advances in Dentistry [Internet]. 2010 Dec [cited 2022 Sep 05] ; 26(6): 295-300. Available in: http://scielo.isciii.es/scielo.php?script=sci_arttext&pid=S0213-12852010000600003&lng=es
2. Tatullo M, Marrelli M, Mastrangelo F, Gherlone E. Bone Inflammation, Bone Infection, and Dental Implants Failure: Histological and Cytological Aspects Related to Cement Excess. J Bone Jt Infect. 2017 Jan 17;2(2):84-89. doi: 10.7150/jbji.17507. PMID: 28529868; PMCID: PMC5423581. (cited Sep 05, 2022). Available in: https://www-ncbi-nlm-nih-gov.translate.goog/pmc/articles/PMC5423581/?_x_tr_sl=en&_x_tr_tl=es&_x_tr_hl=es-419&_x_tr_pto=wapp
3. Cleveland Clinic medical professional. Abscessed Tooth. Cleveland Clinic (Internet). Review on August 24, 2022 (consulted on September 05, 2022). Available on: https://my.clevelandclinic.org/health/diseases/10943-abscessed-tooth
4. Aaron Kandola, Christine Frank, DDS. Signs and symptoms of tooth infection spreading to the body. Medical News Today (Internet). Review on April 03, 2020 (consulted on September 05, 2022). Available on: https://www.medicalnewstoday.com/articles/symptoms-of-tooth-infection-spreading-to-body